Single cell sequencing of HTLV-1 infected individuals to uncover the disease mechanism of adult T-cell leukemia (ATL) and HTLV-1 associated myelopathy/tropical spastic paraparesis (HAM/TSP)
Human T-cell leukemia virus type 1 (HTLV-1) primarily infects CD4+T cells and a small portion of CD8+T cells and prefers long incubation period. ~95% of the infected individuals remain as asymptomatic carrier (AC), 3-5% develop adult T-cell leukemia (ATL) and >1% develop a neuroinflammatory disease, known as HTLV-1 associated myelopathy/tropical spastic paraparesis (HAM/TSP). As the same retrovirus, HTLV-1 causing two different kinds of diseases, it has become very important to study the different disease pathogenesis. In our lab, we aim to use single cell approach to uncover the disease mechanism of ATL and HAM/TSP.
Points
Uncovering ATL disease mechanism by single cell sequencing
Using single cell approach, we showed-
- HTLV-1-mediated leukemic transformation is a seamless transition from physiological T-cell activation where infected cells in an activated state further transforms into ATL cells, retaining its activated phenotype
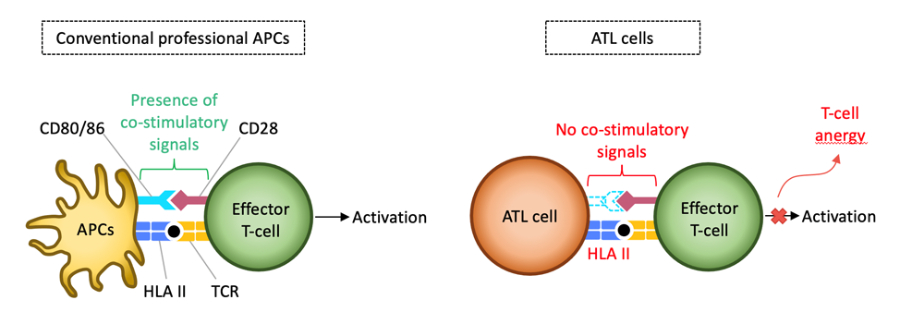
- HTLV-1-infected CD4+T cells upregulate HLA class II molecules; but due to the lack of necessary co-stimulatory molecules used for T-cell activation, these cells instead caused T-cell anergy which allows the infected cells to escape immune surveillance
- Our findings further enhance our understanding on HTLV-1-mediated leukemogenesis and immune evasion which allows us to identify new molecules such as HLA class II as potential targets for immunotherapy
A joint research group led by Prof. Yorifumi Satou at the Joint Research Center for Human Retrovirus Infection, Kumamoto University has completed a single-cell study on HTLV-1 which shed light on how HTLV-1-infected CD4+T cells escape immune surveillance and transform into ATL cells. This research was conducted in collaboration with Dr. Masahiro Ono from Imperial College London. The results were published in the Journal of Clinical Investigation on 2021.
Elucidation of HAM/TSP disease mechanism by single cell sequencing
Currently, our lab is working on the detailed pathogenesis mechanism of HAM/TSP using both PBMC and CSF samples from the patients. We aim to clarify the following-
- From the Asymptomatic carrier stage, which factors facilitates the HAM/TSP development?
- How and why some infected T-cells infiltrates to CSF?
What is the role of infected and uninfected T-cells in the site of inflammation?
Research Overview
In the human body, CD4+ T cells play an important role in regulating the immune response against pathogens and cancers. Upon recognizing foreign/cancer antigen, these cells become activated and carries out its effector functions together with other immune cells in the body to clear the invading pathogens. This is termed ‘physiological T-cell activation/differentiation’.
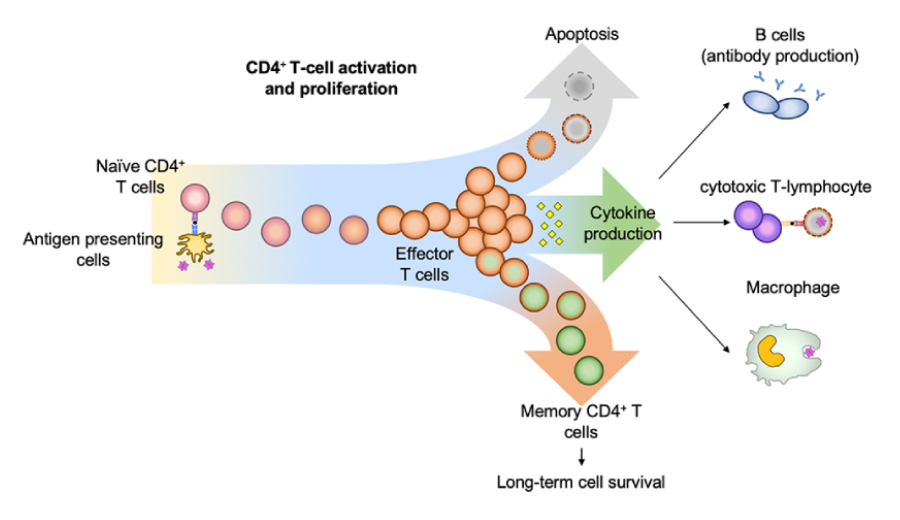
To overcome this barrier, human T-cell leukemia virus type 1 (HTLV-1) infects the CD4+T-cells themselves and causes a specific type of leukemia termed adult T-cell leukemia/lymphoma (ATL). In Japan, there are at least 1.1 million HTLV-1-infected individuals and approximately 1,500 patients are newly diagnosed with ATL every year. Several studies have reported that HTLV-1 can alter CD4+ T-cell differentiation, activation and survival pathways to trigger transformation into ATL. This process is termed ‘HTLV-1-mediated leukemic transformation’. However, the link between physiological T-cell activation and HTLV-1-mediated activation/transformation is still unclear.
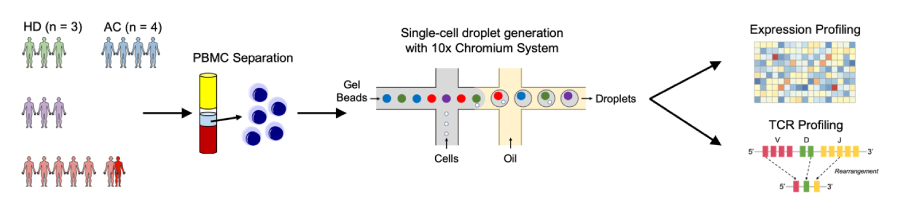
In this study, we applied single-cell RNA-seq (scRNA-seq) to examine immune cells from HTLV-1-infected and healthy individuals at a single cell level. We showed that HTLV-1-mediated leukemic transformation is an extension of the physiological T-cell activation pathway wherein HTLV-1-infected cells in an activated state retain its phenotype and further transformed into ATL cells.
Additionally, HTLV-1-infected CD4+ T cells also upregulate HLA class II molecules. HLA class II, together with the co-stimulatory molecules CD80/CD86, are important surface proteins for T-cell activation. However, HTLV-1-infected CD4+ T cells do not express CD80/CD86 and as such, these cells could not activate T cells but rather induced T-cell anergy or inactivation. This leads to a suppressed immune response which allows the virus and infected cells to escape immune surveillance.
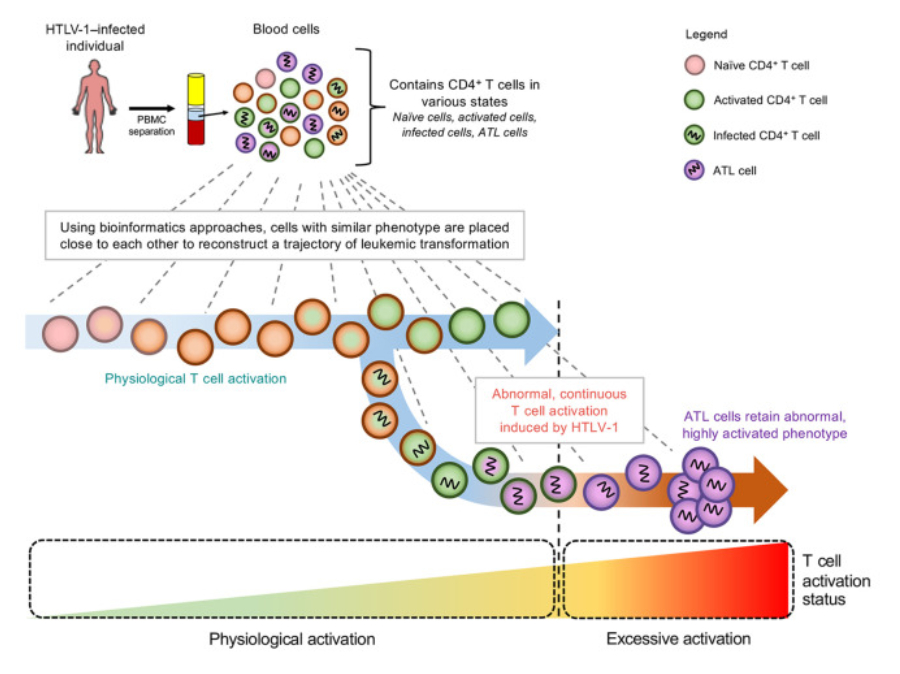
In conclusion, using scRNA-seq, we showed that HTLV-1 exploits the physiological T-cell activation mechanisms for leukemic transformation and demonstrated that by upregulating HLA class II, HTLV-1-infected CD4+T cells are able to escape immune surveillance in the human body. This exemplifies the huge potential of single-cell methods to further improve our understanding on HTLV-1-mediated leukemogenesis and identification of new, potential molecules for immunotherapy.
Publication information
Title:HTLV-1 infection promotes T-cell activation and malignant transformation into adult T-cell leukemia/lymphoma
Authors::Benjy Jek Yang Tan, Kenji Sugata, Omnia Reda, Misaki Matsuo, Kyosuke Uchiyama, Paola Miyazato, Vincent Hahaut, Makoto Yamagishi, Kaoru Uchimaru, Yutaka Suzuki, Takamasa Ueno, Hitoshi Suzushima, Hiroo Katsuya, Masahito Tokunaga, Yoshikazu Uchiyama, Hideaki Nakamura, Eisaburo Sueoka, Atae Utsunomiya, Masahiro Ono and Yorifumi Satou
Journal:Journal of Clinical Investigation
